Vasculitis
Vasculitis is an inflammation of the blood vessels.
Inflammation is a condition in which tissue is damaged by blood cells entering
the tissues. In inflammatory diseases, these cells are mostly white blood
cells. White blood cells circulate and serve as our major defense against
infection. Ordinarily, white blood cells destroy bacteria and viruses. However,
they can also damage normal tissue if they invade it.
Vasculitis can affect:
How Does Vasculitis Damage The Body?
Several things can happen to an inflamed blood
vessel.
Vasculitis can be caused by:
Antigen and antibody bound together are called immune
complexes. Two primary ways in which immune complexes destroy antigens
are:
In these cases, the antigens causing the immune complexes are
often not known. In some cases, the complexes contain DNA and anti-DNA
antigens, or Ro (also called SS-A) and anti-Ro antigens. A recently discovered
antibody, ANCA (anti-neutrophil cytoplasm antibody), can cause vasculitis in
some individuals.
Diseases Associated With Vasculitis
Vasculitis can occur in many different illnesses. Vasculitis
can also occur by itself without any obvious associated infection or other
illness. Some of the illnesses that can cause vasculitis are:
Vasculitis can cause many different symptoms, depending
upon:
occurs include:
Systemic symptoms (this set of complaints can occur in
many illnesses and is not specific to vasculitis)
Skin
Common vasculitis skin lesions are:
Areas of dead skin can appear as:
Joints
Brain
Vasculitis in the brain can cause many problems, from mild to
severe, including:
Peripheral Nerves
Peripheral nerve symptoms may include:
Intestines
Heart
Lungs
Kidneys
Eyes
The diagnosis of vasculitis is based on:
Blood testing
Blood abnormalities that often occur when vasculitis is
present include:
Blood tests can also be used to:
Other laboratory tests
The physician may also order a urine analysis, or
urinalysis.
Heart testing
If there are any symptoms that suggest heart involvement,
tests that may be ordered include:
Lung testing
For lung symptoms, the physician may order:
Abdominal testing
If there are abdominal symptoms, the physician may
order:
Brain testing
For brain symptoms, the doctor may use:
Blood vessel testing
The physician can use a procedure called angiography to see if
there is inflammation in medium and large arteries or veins. This can be done
in any area of the body by injecting dye into the arteries or veins and viewing
the outlines of the blood vessels on x-ray.
Tissue testing (biopsy)
The diagnosis of vasculitis is most firmly made by taking a
biopsy of the involved tissue and examining that tissue under a microscope.
Your physician may suggest this procedure.
Referrals to specialists
Finally,it may be important for your physician to consult
with other medical specialists about your case.
For example,if your physician is a rheumatologist and you
have visual complaints which could be indicative of vasculitis, you may be
referred to an ophthalmologist.
However, it is very important that one physician be in charge
of your case for two reasons:
Treating Vasculitis
The choice of treatment for vasculitis depends on several
factors:
If you suspect that you or a friend or relative has
vasculitis, a physician should be consulted as soon as possible.
Remember:
recognize and treat vasculitis. These include:
Outcome
There are various outcomes for people suffering from
vasculitis.
For the vast majority of people with vasculitis, treatment is
very effective. However:
Inflammation is a condition in which tissue is damaged by blood cells entering
the tissues. In inflammatory diseases, these cells are mostly white blood
cells. White blood cells circulate and serve as our major defense against
infection. Ordinarily, white blood cells destroy bacteria and viruses. However,
they can also damage normal tissue if they invade it.
Vasculitis can affect:
- very small blood vessels (capillaries),
- medium-size blood vessels (arterioles or venules), or
- large blood vessels (arteries or veins).
How Does Vasculitis Damage The Body?
Several things can happen to an inflamed blood
vessel.
- If it is a small vessel, it may break and produce tiny areas
of bleeding in the tissue. These areas will appear as small red or purple dots
on the skin. - If a larger vessel is inflamed, it may swell and produce a nodule which may
be felt if the blood vessel is close to the skin surface. - The inside of the vessel tube may become narrowed so that blood flow is
reduced. - The inside of the vessel tube may become totally closed, usually by a blood
clot which forms at the site of inflammation. - If blood flow is reduced or stopped, the tissues which receive blood from
that vessel begin to die.- For example, a person with vasculitis of a medium-sized artery in the hand
may develop a cold finger which hurts whenever it is used. - Occasionally this can progress to gangrene.
- For example, a person with vasculitis of a medium-sized artery in the hand
Vasculitis can be caused by:
- infection of the blood vessel walls
- This is rare. When it occurs, bacteria, viruses or fungi
infect the blood vessel.White blood cells move in to destroy the infectious agents and damage the blood vessel in the process. - This is a serious condition and requires prompt antibiotic
treatment.
- This is rare. When it occurs, bacteria, viruses or fungi
- an immune or "allergic" reaction in the vessel walls.
- This cause of vasculitis is more common.
- Substances which cause allergic reactions are called antigens.
- Antigens cause the body to make proteins called antibodies which bind to the
antigen for the purpose of getting rid of it.
- This cause of vasculitis is more common.
Antigen and antibody bound together are called immune
complexes. Two primary ways in which immune complexes destroy antigens
are:
- by attracting white blood cells to digest the antigen
- by activating other body substances to help destroy the antigens.
- Unfortunately, some immune complexes do not serve their
purpose of destroying antigens. Instead, they remain too long in the body and
circulate in the blood and deposit in tissues. They commonly accumulate in
blood vessel walls, where they cause inflammation. - It is likely that some white blood cells (cytotoxic cells) which kill infectious agents can also accidentally damage blood vessels and cause vasculitis.
- Unfortunately, some immune complexes do not serve their
In these cases, the antigens causing the immune complexes are
often not known. In some cases, the complexes contain DNA and anti-DNA
antigens, or Ro (also called SS-A) and anti-Ro antigens. A recently discovered
antibody, ANCA (anti-neutrophil cytoplasm antibody), can cause vasculitis in
some individuals.
Diseases Associated With Vasculitis
Vasculitis can occur in many different illnesses. Vasculitis
can also occur by itself without any obvious associated infection or other
illness. Some of the illnesses that can cause vasculitis are:
- systemic lupus erythematosus
- rheumatoid arthritis
- polymyalgia rheumatica
- scleroderma
- Wegener's granulomatosis
- temporal arteritis
- cryoglobulinemia
- erythema nodosum
- tumors
- leukemia
- lymphoma
Vasculitis can cause many different symptoms, depending
upon:
- what tissues are involved
- the severity of the tissue damage.
- Some patients are not ill but notice occasional spots on their skin.
- Others are very ill with systemic symptoms and major organ
damage.
occurs include:
Systemic symptoms (this set of complaints can occur in
many illnesses and is not specific to vasculitis)
- fever
- generally feeling bad (malaise)
- muscle and joint pain
- poor appetite
- weight loss
- fatigue
Skin
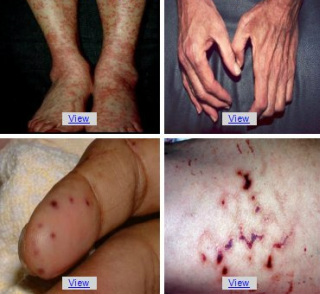
Common vasculitis skin lesions are:
- red or purple dots (petechiae), usually most numerous on the
legs - larger spots, about the size of the end of a finger (purpura), some of which
look like large bruises - Less common vasculitis lesions are hives, an itchy lumpy rash and painful or
tender lumps.
Areas of dead skin can appear as:
- ulcers (especially around the ankles
- small black spots at the ends of the fingers or around the fingernails and
toes (nail fold infarcts) - gangrene of fingers or toes.
Joints
- aching in joints and arthritis with pain
- swelling and heat in joints
- deformities resulting from this arthritis are rare.
Brain
Vasculitis in the brain can cause many problems, from mild to
severe, including:
- headaches
- behavioral disturbances
- confusion
- seizures
- strokes.
Peripheral Nerves
Peripheral nerve symptoms may include:
- numbness and tingling (usually in an arm or a leg, or in
areas which would be covered by gloves or socks) - loss of sensation
- loss of strength (especially in the feet or hands).
Intestines
- Inadequate blood flow in the intestines can cause cramping
abdominal pain and bloating. - If areas in the wall of the intestine develop gangrene, blood will appear in
the stool. - If the intestinal wall develops a hole (a perforation), surgery may be
required.
Heart
- Vasculitis in the coronary arteries is unusual in lupus.
- If it occurs, it can cause a feeling of heaviness in the chest during
exertion (angina), which is relieved by rest. - Heart attacks rarely occur as a result of vasculitis.
Lungs
- Vasculitis in this tissue can cause pneumonia-like attacks
with:- chest x-ray changes that look like pneumonia
- symptoms of fever and cough.
- chest x-ray changes that look like pneumonia
- Occasionally, inflammation can lead to scarring of lung tissue with chronic
shortness of breath.
Kidneys
- Vasculitis is not common in kidneys of people with lupus,
even those who have lupus nephritis. - Vasculitis in the kidneys may not cause any symptoms, although most patients
with renal vasculitis have high blood pressure.
Eyes
- Vasculitis involving the small blood vessels of the retina
can occur in lupus.- The retina is at the back of the eye.
- The cells of the retina have to be activated to form a visual image.
- The retina is at the back of the eye.
- Sometimes, vasculitis of the eyes causes no symptoms. Usually, however:
- There is visual blurring which comes on suddenly and stays.
- A person may even lose a portion of their vision.
- There is visual blurring which comes on suddenly and stays.
- In other non-lupus types of vasculitis, such as temporal arteritis:
- There is sudden loss of part or all of the vision in one eye
- This is usually accompanied by severe headache.
- There is sudden loss of part or all of the vision in one eye
The diagnosis of vasculitis is based on:
- a person's medical history
- current symptoms
- a complete physical examination
- the results of specialized laboratory tests.
Blood testing
Blood abnormalities that often occur when vasculitis is
present include:
- an elevated sedimentation rate
- anemia
- a high white blood cell count
- a high platelet count.
Blood tests can also be used to:
- identify immune complexes or antibodies that cause vasculitis
in the circulation - measure whether complement levels are abnormal.
Other laboratory tests
The physician may also order a urine analysis, or
urinalysis.
Heart testing
If there are any symptoms that suggest heart involvement,
tests that may be ordered include:
- EKG (electrocardiogram)
- ECHO cardiogram
- heart scans.
Lung testing
For lung symptoms, the physician may order:
- a chest x-ray
- blood from an artery to measure the oxygen content
- a pulmonary function test, which uses a specialized machine to measure how
well the lungs handle air and oxygen as you breathe into it.
Abdominal testing
If there are abdominal symptoms, the physician may
order:
- ultrasound or CAT scans of the organs in the abdomen
- special x-rays to see the intestines.
Brain testing
For brain symptoms, the doctor may use:
- CAT scans
- magnetic resonance images (MRI).
Blood vessel testing
The physician can use a procedure called angiography to see if
there is inflammation in medium and large arteries or veins. This can be done
in any area of the body by injecting dye into the arteries or veins and viewing
the outlines of the blood vessels on x-ray.
Tissue testing (biopsy)
The diagnosis of vasculitis is most firmly made by taking a
biopsy of the involved tissue and examining that tissue under a microscope.
Your physician may suggest this procedure.
Referrals to specialists
Finally,it may be important for your physician to consult
with other medical specialists about your case.
For example,if your physician is a rheumatologist and you
have visual complaints which could be indicative of vasculitis, you may be
referred to an ophthalmologist.
However, it is very important that one physician be in charge
of your case for two reasons:
- to coordinate your care
- to help you with decisions.
Treating Vasculitis
The choice of treatment for vasculitis depends on several
factors:
- the severity of the vasculitis
- your general health
- your past reactions (positive and negative) to medications.
- Many cases of vasculitis do not require treatment.
- For example, a few spots on the skin now and then (if not
combined with other symptoms) may not require any medications.
- For example, a few spots on the skin now and then (if not
- Most physicians recommend cortisone-type medications as the initial
treatment for vasculitis., such as:- prednisoneprednisolone
- methylprednisolone (brand name: Medrol)
- Some people with severe vasculitis or vasculitis that does not respond well
to cortisone-type drugs will need to be treated with cytotoxic drugs.- Cytotoxic drugs kill the cells that cause inflammation in the
blood vessels. The two most frequently used are azathioprine (brand name:
Imuran) and cyclophosphamide (brand name: Cytoxan). - Cytotoxic medications are usually used in combination with prednisone and
are often effective in treating vasculitis.
- Cytotoxic drugs kill the cells that cause inflammation in the
- Experimental procedures that have been helpful in treating some cases of
vasculitis include:- plasmapheresisintravenous gamma globulin
- cyclosporin, a medication used to prevent organ rejection in transplant
patients. - Experimental therapies change frequently. Your physician can provide you
with current information.
If you suspect that you or a friend or relative has
vasculitis, a physician should be consulted as soon as possible.
Remember:
- vasculitis can be very mild and of little importance OR
- very severe and life-threatening OR
- any degree in between.
- if you have vasculitis
- if so, how serious it is
- if and how it should be treated.
recognize and treat vasculitis. These include:
- rheumatologists (joints and muscles)
- general internists (the adult body)
- dermatologists (skin)
- hematologists (blood)
- nephrologists (kidneys)
- gastroenterologists (the intestinal tracts, stomach, etc.)
- infectious disease experts
- pulmonologists (lungs)
- cardiologists (heart)
- geriatricians (the elderly)
- neurologists (the nervous system)
- ophthalmologists (the eyes).
Outcome
There are various outcomes for people suffering from
vasculitis.
- For many patients, vasculitis, especially if confined to the
skin, may be annoying but never life-threatening. For those individuals, life
can be normal -- or close to it. - On the other hand, a small number of people have severe vasculitis involving
major organ systems. In these cases, damage can occur so rapidly that treatment
does not have time to work or the condition may be resistant to treatment. An
attack of vasculitis can be fatal or permanently disabling for affected
individuals.
For the vast majority of people with vasculitis, treatment is
very effective. However:
- the vasculitis may disappear only to reoccur later and
require treatment again OR - the vasculitis may be suppressed but never really go away, so that some
ongoing treatment is always required.
